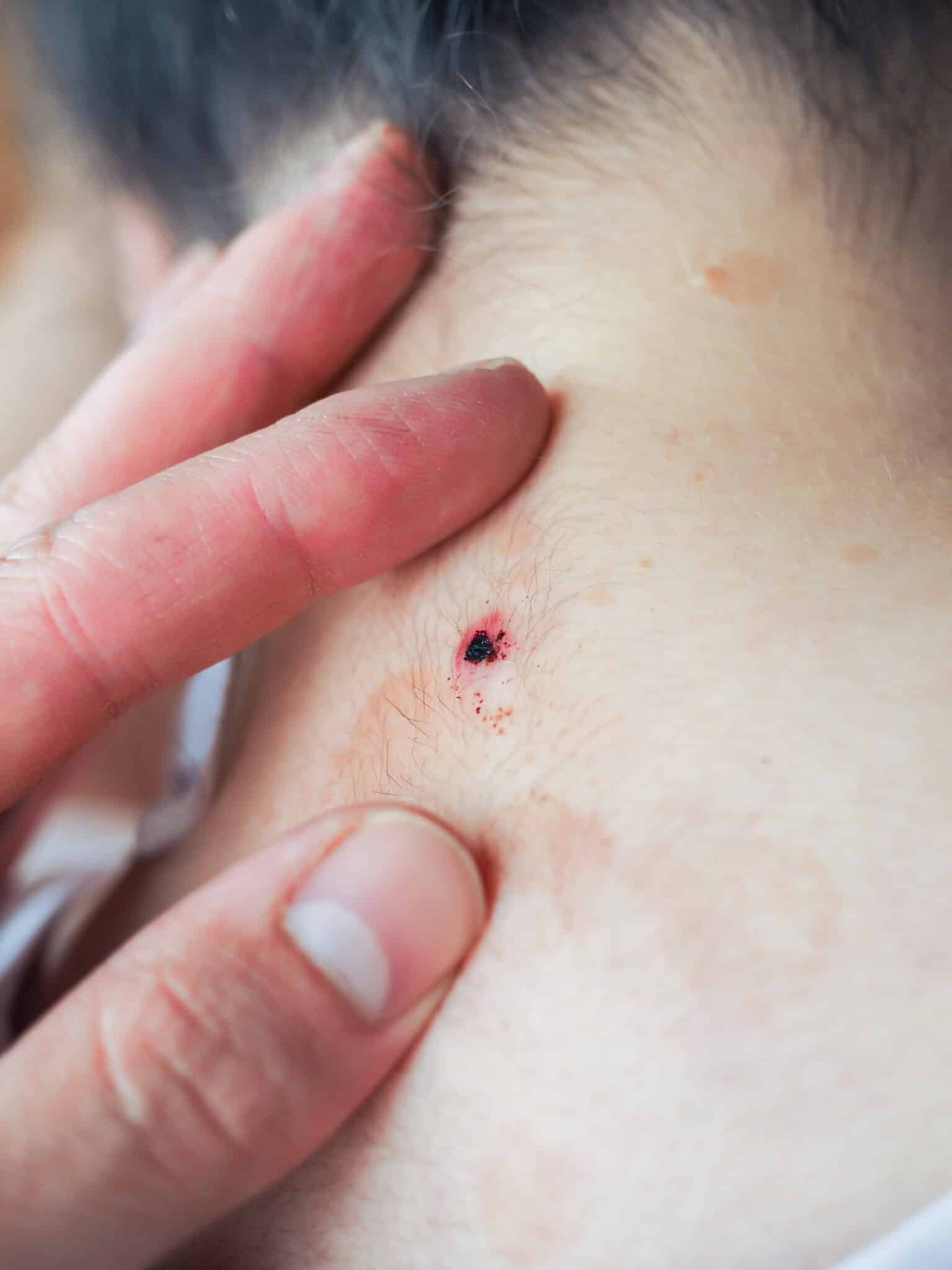
Keloids can sometimes develop after mole removal wounds heal. This is not unique to mole removals, as keloids result from an abnormally excessive healing process that can occur after any skin injury or inflammatory process.
With mole removals, we're usually more concerned with the possibility of sunken scarring but raised hypertrophic or keloid scarring can also develop.
From my experience over the years performing mole removals, the vast majority of the resulting wounds do not develop keloid scarring. However, a small percentage of cases do end up having some form of keloid scarring. I've noticed that certain types of mole removals have a higher chance of such complications.
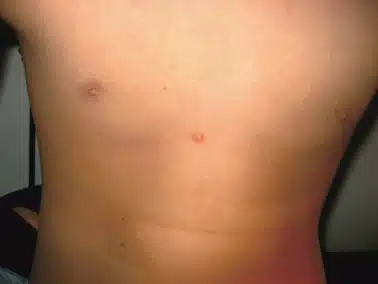
One of the risk factors I've noticed is the location of the mole removal. Most of the more removals I perform are on the face and these usually heal fine without any keloid scarring. However, where there is a lot of stretching, movement, or tension, this seems to contribute to the development of hypertrophic wound healing. Examples include areas around the:
The amount of healing that the skin has to do after mole removal is also a significant factor in the development of subsequent keloid scarring. The deeper and bigger the mole, the more missing tissue the skin has to grow back, increasing the risk of an over-reaction.
However, it's not like you can choose where to develop a mole, or how deep and big it is. So there's really nothing you can do to change or modify this except remove unwanted moles as soon as possible while they are still relatively small and/or shallow.
While you cannot control how deep or big your mole is, one thing you can control is the method used to remove it. Different mole removal methods vary in the amount of collateral damage. Advanced mole removal methods are much more precise, allowing complete removal of the mole tissue with minimal damage to healthy skin tissue.
Less advanced mole removal methods, while they may be fast, simple, and affordable, often result in unnecessary damage to the surrounding tissue. This can lead to an elevated risk of hypertrophic scarring. In fact, I've seen some patients develop keloid scars after mole removals using more rudimentary methods in the hands of less experienced or qualified personnel.

Topical treatments, such as retinoids, silicone-based products, and hydrocolloid dressings are essential for reducing the chance of keloids developing after mole removal. While they are research-backed and have a definite positive effect, the magnitude of that effect is not as strong as the injectibles in my experience. Nevertheless, I would recommend them as they are generally safe and well-tolerated.
Injectibles have a bigger effect on the final outcome of the scarring after mole removal than topicals. I would say that short of the actual mole removal technique used, injectibles have the biggest impact on whether or not a keloid scar develops after the wound heals.
Growth factors help during the wound healing phase by speeding up wound closure and exerting an anti-inflammatory effect. This reduces the chances of an excessive healing response that may lead to hypertrophic or keloid scarring.
Injectibles used for keloid treatment can also be used to reduce the chance of a keloid developing. Steroids are commonly available however they have to be used very carefully. Trying to prevent keloid scarring with steroids is risky. Overzealous or incorrect treatment may instead result in an atrophic or sunken scar that is then even more difficult to rescue. Other injectibles may work better as they interfere less with the healing process and have a lower risk of causing skin atrophy. My personal favourite injectible for keloid prevention after mole removal is neurotoxin. Neurotoxins, while more costly, have the advantage of not affecting the healing process and minimal side effects.
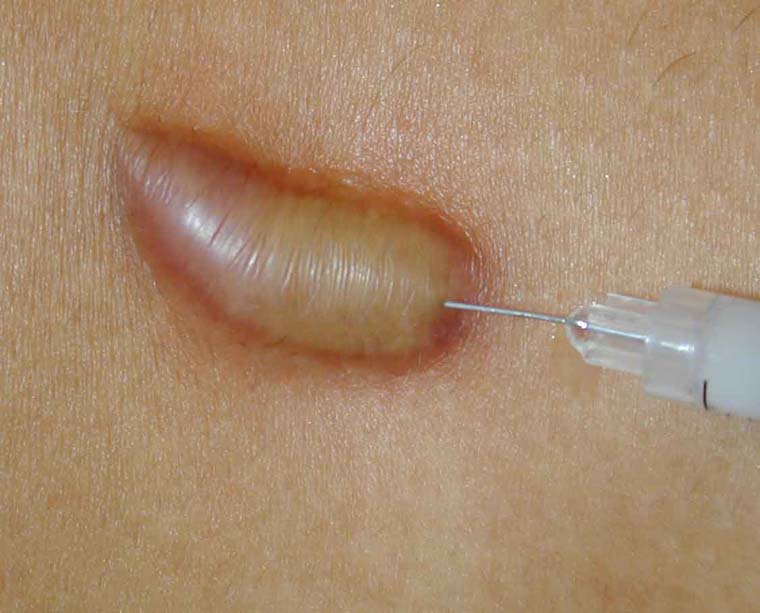
Sometimes, despite our best efforts to apply all the right preventive measures, a keloid can still form after mole removal.
Thankfully, from my experience, such keloids generally respond very well to treatment. The key is to spot abnormal wound healing and institute the appropriate treatment early, as the keloid will respond better and faster to early treatment. Most of the time, we are able to flatten out the keloid and suppress the over-exuberant healing with injectibles.
Most of the time, keloid scar removal surgery is not necessary unless the keloid is very large, mature, or resistant to treatment.
While mole removal does not often result in keloid scars, they can and do develop. We should proactively take evidence-based measures to reduce the chance of keloids developing. This is especially important in moles where there is an elevated risk of keloid development after mole removal. We should also be mindful of the importance of monitoring and early treatment.
Mole removals and keloid scar treatments are two of the more common treatments that we do. I hope that my perspective has given you some insight into the topic. Please let me know if I can answer any other questions. If you have a mole removal in mind but are worried about keloids, or have developed a keloid after mole removal, please feel free to schedule a consultation and we'll do our best to address your condition holistically.
Address:
1Aesthetics, Medical & Surgery
#14-90 The Central Tower 1
8 Eu Tong Sen Street
Singapore 059818
Mon-Fri 10 AM to 730 PM
Sat 10 AM to 6 PM
Phone / WhatsApp:
+65 66125173 / +65 84899962
Email:
info@1aesthetics.com