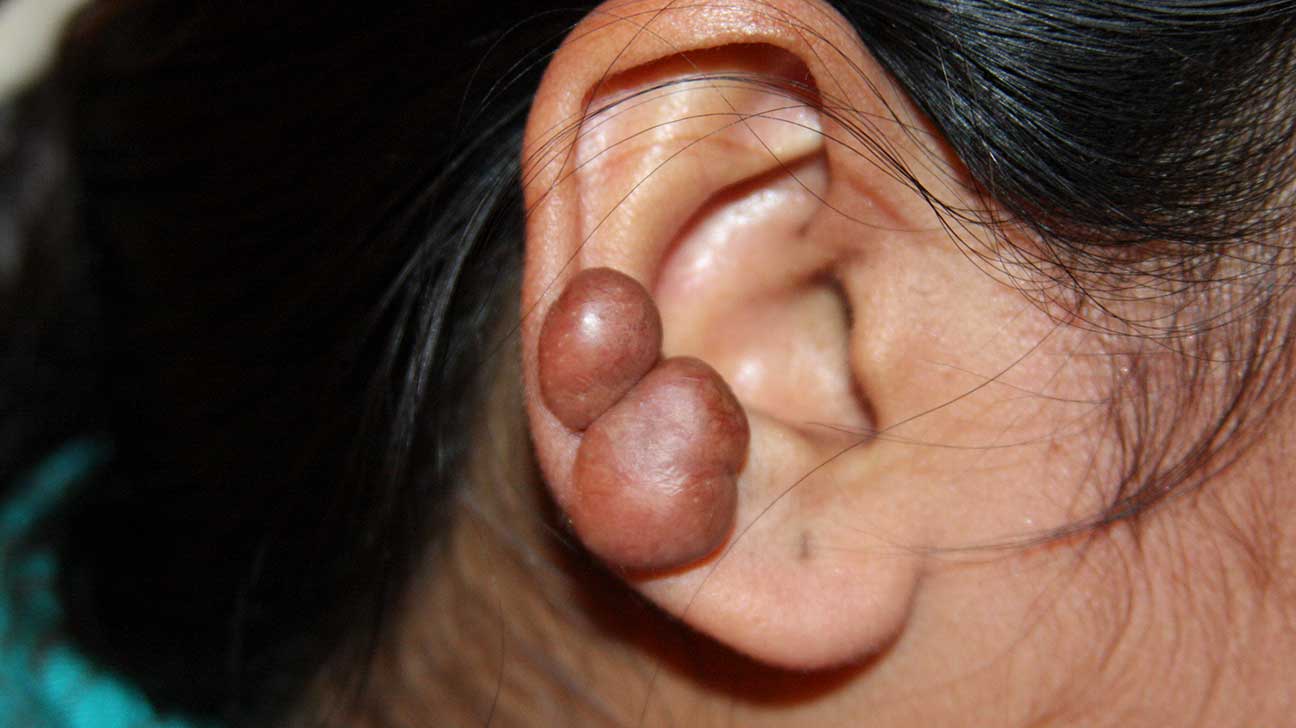
Many medical aesthetics, plastic surgery, dermatology, and even GP clinics in Singapore offer keloid scar removal treatment. Keloid injections are the first-line and probably the most common form of intervention offered in Singapore clinics.
The most widely available and administered keloid injections in Singapore are intralesional steroids. Steroids induce keloid regression through many different mechanisms such as suppressing inflammation, constricting blood supply, inhibiting cell division, and reduced collagen production.
Steroid injections may cause complications such as the formation of new blood vessels, pigmentary changes, thinning of the skin, subcutaneous fat or even underlying tendons or bone, or even skin necrosis and ulcerations. They may also cause problems elsewhere in the body such as acne flares or Cushing’s syndrome.
I have personally treated a patient who developed sunken scarring from a deep ulcer on the cheek from a steroid injection gone wrong. She had gone to another clinic for cystic acne and received a cortisone injection for acne. Unfortunately, the skin broke down into a deep wound. Thankfully she came to us for scar removal treatment early and we were able to flatten out the scar with growth factors and fractional lasers. Thus, steroid injections have to be done with the utmost care, paying attention to the depth, amount, concentration, and angle of injection.
One of the key questions that I get asked frequently is: Does the keloid injection hurt?
Steroid injections for keloid scar removal are typically quite painful. This is because of what is inside the keloid - the thick fibrous keloid tissue is very difficult to inject into. Some patients dread or even discontinue treatment because of this. I've developed some techniques to greatly reduce the pain from the injection.
The cost for steroid injections has also risen over the years, with a particularly pronounced jump after an orthopedic specialist was fined $100,000 after a patient developed complications after a steroid injection (for a non-keloid condition) that lead many doctors to avoid performing steroid injections for fear of being sued or hefty malpractice insurance premiums. Intralesional steroid injections for keloid treatments used to start from $50-100 years ago but the costs have increased a few times at least, now ranging from $150-200 up to a few hundred dollars or even more.
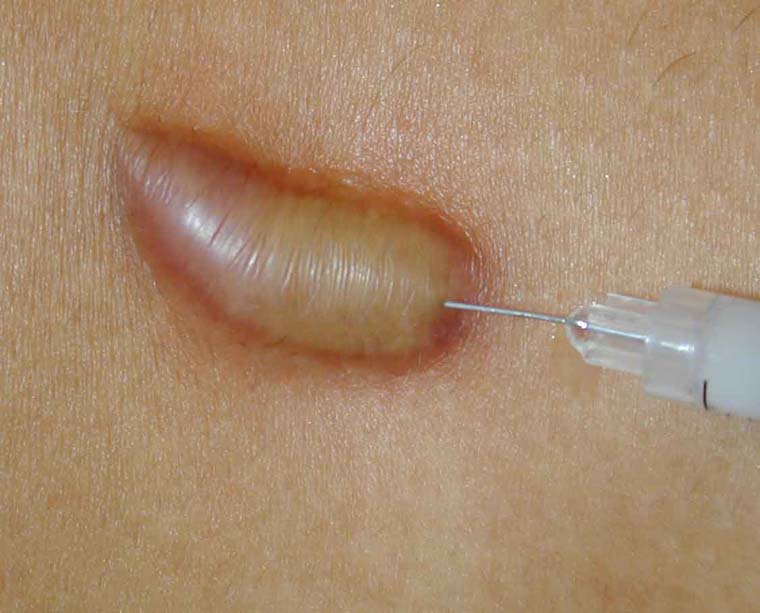
Antimetabolites such as pyrimidine analogues can block collagen synthesis, reducing fibroblast activity. The reduction in keloid volume (flattening, decrease in length and width), decrease in itching, and recurrence rate appeared to be comparable to steroids. However, side effects (such as pain, hyperpigmentation, and ulceration) were significantly more common.
Water-soluble glycopeptide antibiotics can induce apoptosis and reduce TGF-β1-induced collagen synthesis. Side effects include pain, superficial ulceration and crusting at injection sites, transient hyperpigmentation, and dermal atrophy.
Commonly used calcium antagonists can increase collagen degradation. Intralesional calcium antagonists had a lower complication rate but were slower, less effective, and had higher recurrence rates than steroids.
Intralesional neurotoxin injections may improve and prevent hypertrophic scars and keloids by suppressing scar tension and fibroblast activities. Tension is one of the causes of keloid scars. Neurotoxins reduce tension on the wound edges by preventing muscle contraction during healing, thereby reducing scar formation. In one study, intralesional neurotoxin injections improved keloids and decreased keloid volume more effectively than intralesional corticosteroid injections.
Unlike most injectable keloid treatments, neurotoxin injections are relatively benign and are less likely to have serious side effects. However, neurotoxins cost significantly more than steroids, and relatively large amounts have to be used. Hence neurotoxin injections for keloid treatment can cost double or more compared to intralesional steroid injections.
Generally, keloid injections are considered safe, with a positive risk-benefit ratio when administered by a qualified doctor in appropriate dosages and under proper conditions. However, like all medications, keloid injections carry some risks and potential side effects. My experience is that neurotoxins are much safer than steroids in terms of the risk of complications.
Steroid injections are indispensable to keloid scar removal treatment. While well-researched and effective, drawbacks include the potential for severe side effects, pain, and cost. Combination treatment with other injectable medications has been shown to improve response and reduce side effects. However, most alternative treatments are expensive and difficult to find in Singapore as most clinics would not stock these due to the low volume and high cost. Furthermore, they may have even higher complication rates than steroid injections.
Personally, I find neurotoxins to be a valuable addition to the range of treatments we have for keloid scar removal treatments. Firstly, we already stock neurotoxins for medical aesthetics treatments like anti-ageing and wrinkle reduction treatments. Secondly, the risk of side effects is low compared to steroid injections. Lastly, its mechanism of action is different from steroid injections, providing some synergy and a better, faster response to treatment.
Combination injections are also an essential part of other keloid removal treatments such as vascular lasers, or advanced keloid removal surgery.
Keloids are undoubtedly difficult to treat but it is not impossible — especially in the hands of an experienced doctor. Successful keloid removal treatment, while harder than you might expect, can produce gratifying and dramatic results from the right treatment regimen. If you're suffering from a keloid and frustrated at just being treated with steroid injections, book a consultation with us today.
Here's to a keloid-free life!
Address:
1Aesthetics, Medical & Surgery
#14-90 The Central Tower 1
8 Eu Tong Sen Street
Singapore 059818
Mon-Fri 10 AM to 730 PM
Sat 10 AM to 6 PM
Phone / WhatsApp:
+65 66125173 / +65 84899962
Email:
[email protected]