
Today, we will delve deeper into a topic that is often misunderstood and overlooked: keloid scar removal surgery.
The term “keloid” itself was first used in the 19th century by the French dermatologist Alphonse Devergie, but the condition has been recognized for thousands of years. Keloids are large, thickened, and raised red growths that result from an abnormal healing response. They are characterized by an exuberant inflammatory reaction to injury and subsequent excessive collagen deposition. Keloids can develop after any sort of skin injury, including acne, ear piercings, tattoo or mole removals, accidental burns and abrasions, and surgical wounds.
Keloid surgery has a long history, dating back to ancient times. The exact date of the first keloid surgery is not well-documented in medical literature. However, surgical removal of keloids has been practised for centuries.
In the past, treatment options for keloids were limited and often ineffective. Traditional methods of keloid removal included simple surgical excision, which often resulted in the keloid returning larger than before. This is because the process of healing from the surgery could trigger the overgrowth of keloidal scar tissue.
Over time, medical understanding of keloids and their treatment has evolved significantly. Researchers discovered that keloids are not just a simple overgrowth of scar tissue. Instead, it is a complex condition involving an abnormal response to skin injury, with genetic factors playing a role.
This understanding led to the development of new surgical techniques aimed at not just removing the keloid, but also addressing the underlying factors that cause keloid formation. These include techniques such as extramarginal excision and fillet flap excision.
Unlike surgeries for lumps and bumps such as lipomas, keloid scar removal surgery is not intended to instantly cure keloids. The intent of keloid removal surgery is to debulk the keloid, especially those that are mature, stubborn, and resistant to non-surgical therapy. Once the keloid core has been removed, other treatments that thoroughly suppress the excessive healing response can then follow.
No, not all keloids need to be surgically removed. The decision depends on several factors, including the keloid's size and location, whether it’s causing discomfort or pain, and the patient’s personal preferences.
Some keloids may be effectively managed with non-surgical treatments such as corticosteroid injections, laser therapy, or topical treatments. These can help to flatten keloids and reduce their redness, itching, and pain.
However, in some cases where the keloid is large, causing significant symptoms, unlikely to respond or not responding to other treatments, surgical removal may be considered. If you’re considering keloid removal surgery, please read this article on our website to see if your keloid is suitable for treatment.

Many doctors advise against operating on keloids, saying it’s not possible to have a good outcome and the keloid will only grow back worse. However, this really depends on surgical technique and adherence to keloid suppression after surgery.
In published studies, the recurrence of keloids was closely related to the method for coverage of the defect after surgical excision. The “5 As and one B” (asepsis, atraumatic technique, absence of raw surface, avoidance of tension, accurate approximation of wound margin, and complete bleeding control) are important factors in reducing the recurrence rate of earlobe keloids in surgical excision.
Advanced techniques can nowadays minimize the amount of healing/inflammation and hence the risk for recurrence or worsening of the keloids.
Shave surgery involves literally shaving off the protruding portion of the keloid. In the past, this used to be done with cold steel. With advancements in technology such as ablative or vascular lasers, shave surgery has become more precise and less invasive. The drawbacks of this method are that it will not remove deep-seated keloid scar tissue, and the large raw surface takes a long time to heal. This produces a lot of inflammation that stimulates keloid regrowth and worsening.
Extramarginal excision is a surgical technique favoured by plastic surgeons for the removal of keloids. It involves surgically removing the entire piece of skin containing the keloid and suturing the surrounding skin together. This technique aims to completely remove the keloid, including its margins, to prevent recurrence. Since the surrounding skin is stretched to close the wound, the suture line is subject to a lot of tension that stimulates keloid growth. To counteract this tension, methods such as subdermal antitension sutures have been devised. These sutures are placed beneath the skin to distribute tension across a wider area, reducing stress on the wound edges.
Other plastic surgical techniques such as z-plasty, grafts, and flaps can also be used in conjunction with extramarginal excision. Z-plasty is a method of redistributing tension on a wound by creating zigzag patterns with flaps. Grafts involve taking skin from another part of the body to cover the wound, while flaps refer to moving the skin along with its blood supply from a nearby or distant area to cover the wound. However, these techniques often result in bigger or more scars. Therefore, it’s crucial to weigh the potential benefits against the risks. Discuss these factors thoroughly with your surgeon before deciding.
Despite these challenges, extramarginal excision can be effective when combined with other treatments such as corticosteroids, other keloid injections, or radiation therapy.
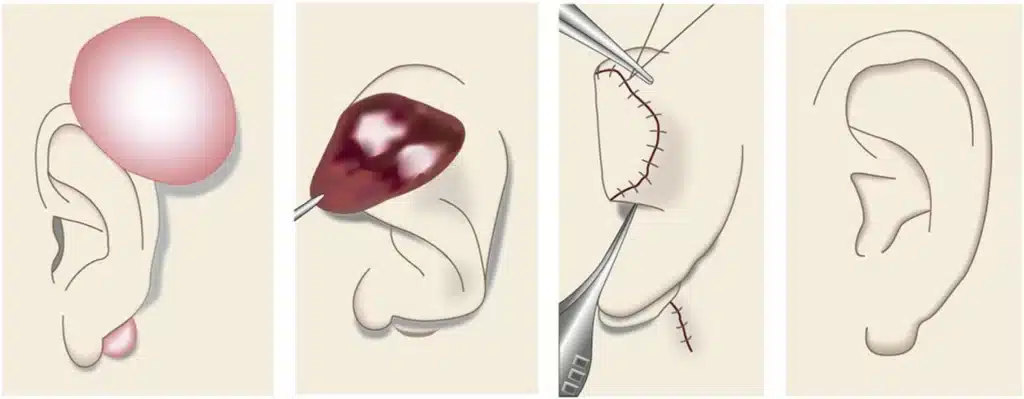
Fillet flap excision is a type of surgery that involves incising the keloid and removing its core under direct vision while preserving intact skin flaps. This technique, termed a “keloid fillet flap,” is performed under local anaesthesia. The skin over the keloid is dissected from the keloid mass as a flap, and the keloid mass is completely removed. Subcutaneous sutures are not used. The keloid fillet skin flaps are then used to close the wound with 6-0 non-absorbable sutures after trimming.
It requires surgical skill including dissecting and removing the keloid from the overlying skin that will act as the “flap” used to cover the wound after removing the keloid.
The fillet flap technique has several advantages, albeit undermined by some technical difficulty in fully removing the hard, fibrotic keloid tissue, especially in smaller keloids where there is a higher risk of accidental damage to the thin roof layer which will constitute the flap. Furthermore, there may be issues with healing at the incision in large or extensive keloids.
The minimally invasive version of fillet flap excision uses much tinier incisions that heal better but it requires more technical finesse since the entire surgery is without direct vision of the keloid scar tissue. However, in larger keloids, the success rate and flap survival are far superior to regular fillet flap excision.
No, keloid surgery actually doesn't hurt as much as you might think it does. In fact, keloid surgery may even hurt less than non-surgical treatments such as keloid injections or lasers. This is because the area to be operated on will be completely numb after local anaesthesia. Generally, the operated area will not be very painful after surgery either.
The duration of a keloid surgery can vary widely depending on several factors, including the size and location of the keloid, the specific surgical technique being used, and whether any adjunctive treatments are being applied during the procedure.
For example, a simple shave excision of a small keloid might take only 15-30 minutes, while a more complex procedure like an extramarginal excision or a fillet flap excision for a large keloid could take several hours.
After any type of surgical procedure for keloid removal, it’s crucial to follow post-operative care instructions diligently. This may include applying silicone gel or other keloid topical creams, using a pressure device, or following up with lasers, intralesional steroids, or other injections.
Keloids can be challenging to treat due to their unpredictable nature and high recurrence rate. However, it’s possible to effectively manage these stubborn scars with advancements in surgical techniques and post-operative care strategies. Remember: every individual case is unique, so it’s important to consult with a medical professional who can provide personalized advice based on your specific situation.
At 1Aesthetics, we’re committed to providing safe and effective treatments for various skin conditions including keloids. If you have any questions or would like to schedule a consultation, please don’t hesitate to contact us. We’re here to help you on your journey towards healthier skin.
Address:
1Aesthetics, Medical & Surgery
#14-90 The Central Tower 1
8 Eu Tong Sen Street
Singapore 059818
Mon-Fri 10 AM to 730 PM
Sat 10 AM to 6 PM
Phone / WhatsApp:
+65 66125173 / +65 84899962
Email:
[email protected]