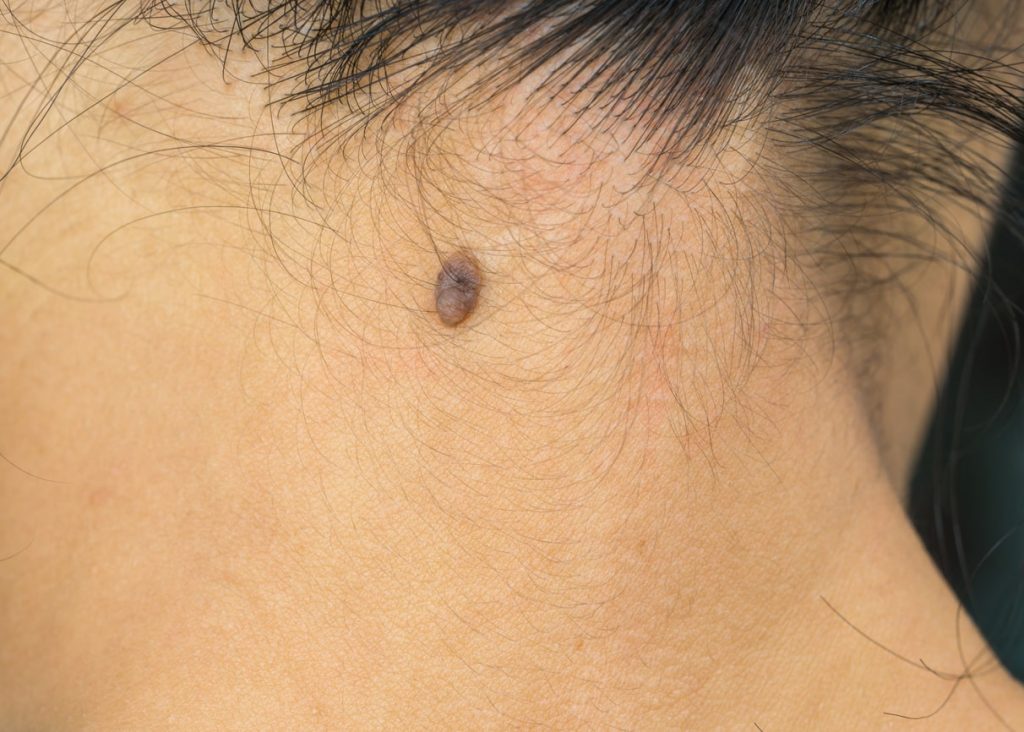
Are you considering mole removal? If so, you may be wondering about the chances of your mole growing back after removal.
Mole removal is a common procedure. While mole removal is often permanent, it is not impossible for a mole to grow back and even increase in size after it has been removed. Several factors determine the likelihood of mole recurrence, including the type of mole, its nature (benign or malignant), the method of removal, your skin's healing process, and the skill and experience of the surgeon.
Moles, medically known as nevi (singular: nevus), are visible, circumscribed, and chronic lesions that can be found on the skin or mucosa. They can appear similar to other common skin lesions such as skin tags, freckles, and seborrheic keratosis. Moles may develop from melanocytes, which are cells that make a pigment called melanin. Melanin gives our skin and hair their natural color and protects our body from ultraviolet (UV) radiation. As people with lighter skin have less natural protection from UV, they are more likely to develop new moles after exposure to the sun. In addition, their moles tend to be darker too.
Most moles are benign and are usually pink, brown, or tan with distinct borders. People with lighter skin are more likely to develop new moles after exposure to the sun, and their moles tend to be darker. The most common types of benign moles are:
Atypical moles, or dysplastic nevi, is the term used to describe unusual-looking moles. By unusual, we mean that they are:
Atypical moles are often mistaken for melanoma or cancerous moles. But they are not necessarily cancerous or precancerous. With that said, a dysplastic or atypical nevus has a higher chance of developing into melanoma.
Certain things can cause the appearance of moles to change over time, such as hormonal changes during pregnancy and exposure to sunlight. These changes usually include the darkening or development of new moles. It is good to familiarise yourself with the lesions on your body so you would know if any change is normal or not. If a mole becomes dysplastic, it might be a sign that it has developed melanoma. You should definitely get your mole evaluated as soon as possible.

There are many methods of mole removal available in Singapore, including really cheap mole removal options which I highly discourage as they are ineffective. Some of the methods that are recognized as legitimate options by doctors are:
Through this procedure, the mole is gently shaved off with a surgical blade by a surgeon. No stitches are required and the wound heals in about 1-2 weeks. Shave excision tends to be less precise than other mole removal methods, resulting in an increased risk of recurrence.
Surgical excision removes the entire piece of skin containing both the mole and its ‘root'. This ensures the removal of every part of the abnormal mole cells and that the mole is unlikely to grow back. Surgical excision is usually performed on larger, recurrent, or suspected cancerous moles. However, this procedure will leave a linear scar that is inevitably longer than the diameter of the mole itself. Depending on how well the surgeon repairs the wound and your healing ability, the scar may be a barely visible white line. However, it is not uncommon for the scar to be noticeable.
Laser mole removal is common for aesthetic purposes. The laser uses controlled pulses of light energy to break up the pigment of the mole or vaporize the mole cells. Laser mole removal is much more precise and selective than manual methods hence it can remove mole cells more selectively with less collateral damage.
Laser can be used to vaporize a mole layer-by-layer starting from the surface inwards, to dissect out a mole (as part of microsurgery) or to cut around a mole during surgical excision.
With every procedure, it’s hard to 100% predict if the removed lesion will grow back — the same goes for moles. Generally, if a mole has been removed completely without any cells left behind, it should not grow back. This is especially important for cancerous moles removed by surgical excision; it is vital to eliminate all cancerous cells. Thus, the surgeon would usually remove a wide margin around the cancerous mole to reduce the chance of recurrence, even though doing so would result in more obvious scarring. However, in benign moles, a finer balance needs to be struck between recurrence and scarring.
If a mole grows back after mole removal, it doesn't mean that the mole is definitely cancerous. Most moles that regrow are actually still benign. However, the fact that the mole has regrown does raise the index of suspicion that the mole is cancerous. The regrown mole has to be carefully assessed by the doctor, taking into account factors such as the original appearance of the mole, the findings during the mole removal, the appearance of the regrown mole and the speed of the regrowth.
If the doctor isn't reasonably comfortable that the regrowth is benign or if there are some suspicious features, it is safer to treat the mole regrowth as potentially cancerous. Destructive procedures such as radiofrequency or laser vaporization should be avoided. Instead, the regrown mole should be carefully removed and sent for histological examination to verify if it is benign or malignant.
Recurrence is unlikely after surgical excision. However, while shaving or laser mole removal is a simpler procedure with a lower risk of scarring, there is a possibility that the mole may regrow. This is because the treatment does not remove the entire area of the involved skin, and thus may not completely eliminate all mole cells, leaving some behind that can grow back.
Studies show that shave excision may have a recurrence rate of between 11% to 33%.
The odds of the mole growing back after laser mole removal are much lower than that of shaving but higher than surgical excision. Compared to both of these methods, it can achieve a superior balance between the risk of mole recurrence vs the risk of significant scarring. Of course, there are many types of lasers for mole removal on the market. Ultimately, the outcome rests on the skill of the doctor who performs the procedure, the type of laser used, and how the laser removes the mole.
In one study published in the British Journal of Dermatology, ruby pigment laser was very successful at removing superficial flat brown moles (junctional nevi) within 1-3 sessions with no recurrence after a year of follow-up. However, red-brown, thicker, or even slightly elevated moles did not respond well to laser removal with this laser.
Another study showed no recurrences in moles treated with a combination of ablative and pigment lasers after 6 months of follow-up.
Overall, the chances of benign mole regrowth after removal are higher for younger patients with darker skin types, raised or deeper moles, moles involving hairs or other adnexal structures, and moles with multiple colours.
The timing of the recurrence depends on various factors, including the type of mole and the method of removal. In general, if a mole does grow back, it's usually within the first six months after removal. However, depending on whether it grows towards to skin surface, or remains embedded in the deeper layers, you may only notice it much later.
Scar tissue has a poorer blood supply and weaker healing ability than normal skin tissue. Thus, repeat removal of a mole recurring within scar tissue is more prone to further scarring. This is why I often encourage patients seeking mole removal to go for the method with the best chance of removing the mole without leaving significant scarring at the outset, instead of trying cheaper methods that may result in the mole regrowing within scar tissue.
In conclusion, the chances of mole recurrence after removal depend on various factors such as the type of mole, its location, and the method of removal. Surgical excision is the most effective method for removing melanocytic nevi and reducing the risk of recurrence but at the cost of a surgical scar. Laser mole removal is a popular method of removing moles due to its many benefits but it may not be suitable for all types of moles, and the risks of recurrence may be higher than with surgical excision. It is important to have a benign mole that regrows after removal evaluated by a qualified specialist to determine if it is truly benign or cancerous. If there is any doubt, treat recurrent moles as potential cancers.
If you have a pesky mole that just refuses to go away, get in touch with us and we'll see what we can do!
Address:
1Aesthetics, Medical & Surgery
#14-90 The Central Tower 1
8 Eu Tong Sen Street
Singapore 059818
Mon-Fri 10 AM to 730 PM
Sat 10 AM to 6 PM
Phone / WhatsApp:
+65 66125173 / +65 84899962
Email:
[email protected]