Warts, pesky skin growths caused by the human papillomavirus (HPV), are unsightly and a source of discomfort and embarrassment. Traditionally, wart removal involved physically removing the wart tissue from the skin, often involving destructive methods like freezing, burning, or cutting. While effective, these methods have significant limitations, including scarring, recurrence, expense, and downtime.
Patients are sometimes hesitant to do anything invasive and often ask us: Is there an injection to stop warts? Do wart injections work? Yes, there are indeed wart removal injections that work well to stop warts. In this comprehensive guide, we will delve into this alternative approach, exploring what they are, the types available, and their advantages and drawbacks, to help you make an informed decision about wart removal.
The traditional approach to wart removal involves physically destroying the wart tissue using various methods:
While these methods can be effective, they have notable limitations.

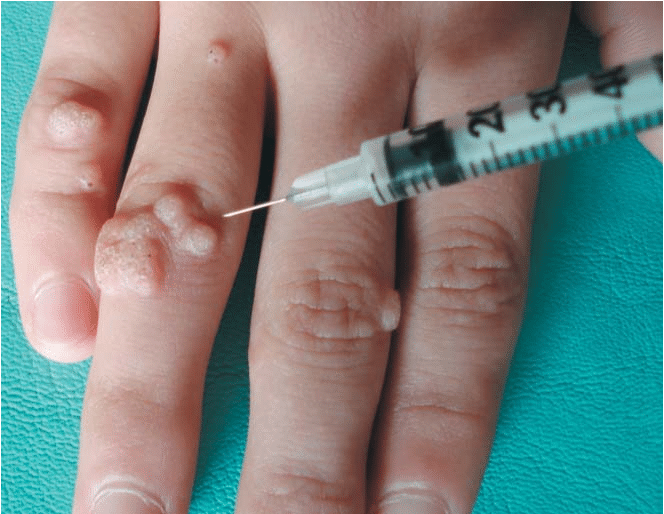
Wart removal injections offer an alternative treatment option. These injections work by either damaging the wart tissue or stimulating the body’s immune system to fight off the wart.
Various chemotherapeutic agents such as pyrimidine analogues and glycopeptide antibiotics have been shown to work for wart removal by damaging wart-infected cells.
Pyrimidine analogues are antimetabolite drugs that inhibit DNA and RNA synthesis, suppressing cell division via cell cycle arrest, and decreasing epidermal proliferation, thus helping in decreasing the proliferation of wart tissue. Studies show success rates of 38-82%.
Cytotoxic glycopeptide anti-neoplastic antibiotics have antitumor, antibacterial, and antiviral activity that inhibits DNA synthesis through DNA strand breakages, preventing cell replication and causing acute wart tissue death. Numerous reports in the treatment of recalcitrant warts show success rates ranging from 14% to 99%.
Cell-mediated immunity plays a major role in wart resolution. Immunotherapy has shown promising potential in treating warts, even in cases of widespread distribution. Extensive research has examined the use of intralesional injections containing vaccines and organic antigens as a wart removal strategy, yielding varying degrees of success.
Although the precise mechanism remains not fully elucidated, these injections are believed to initiate a systemic T-cell-mediated response. This response increases cytokines, particularly those released by Th1 cells, such as interleukin-2, 4, 5, 8, and interferon-gamma. These cytokines play a pivotal role in activating cytotoxic and natural killer cells, which work to eliminate HPV infection.
Immunotherapy for warts addresses the limitations of traditional ablative therapy by the fact that it enhances cell-mediated immunity and enables the body's immune system to clear the virus-infected tissue irrespective of whether they are visible or not. This not only leads to the clearance of local warts but also distant warts, setting immunotherapy apart from traditional wart treatment methods; and making it a preferred option in multiple warts, warts on inaccessible or difficult-to-treat sites (like sub- or peri-ungual regions) or in cosmetically sensitive areas (facial warts).

Vitamin D3 injections for wart removal enhance innate immunity through the production of Defensin B2 and Cathelicidin antimicrobial peptides. They increase antimicrobial chemotactic, autophagic, and phagocytic capabilities in cells like macrophages, monocytes and keratinocytes, ultimately aiding in the elimination of viral-infected keratinocytes. Although the exact mechanism is not fully understood, vitamin D3's role in regulating proliferation, differentiation of epidermal cells, and cytokine production contributes to its effectiveness in wart removal by promoting the elimination of infected cells.
MMR stimulates both cell-mediated and humoral immunity, leading to accelerated viral clearance. Studies have shown its effectiveness in reducing the size of warts and achieving complete resolution in a significant percentage of cases, with some studies reporting up to 63-87% complete resolution. Side effects typically include pain, itching, erythema, and flu-like symptoms.
Candida was the first injectable antigen to be reported as a successful option in the treatment of warts. Intralesional Candida antigen immunotherapy may upregulate macrophage migration inhibitory factor (MIF) and induce specific and non-specific Th1 inflammatory reactions against HPV papillomavirus capsid protein L1. Studies report up to 56-81% success.
PPD contains mycobacterial antigens that upregulate interleukin-2 (IL-2), IL-4, IL-5, and interferon-γ (IFN-γ), inducing a Th1-mediated immune response. Success rates range from 52 to 77%.
Reported side effects of chemotherapy-based wart removal injections include burning during injection, pain, swelling, redness, peeling, crusting, and scab or ulcer formation. Less commonly, there may be complications like hyper- or hypopigmentation, scarring, pneumonia-like symptoms, Raynaud’s phenomenon, and anaphylaxis.
Immunotherapy-based wart removal injections have milder side effects such as pain, itching, redness, swelling, fever, fatigue or other flu-like symptoms.
Chemotherapy-based wart removal injections tend to be more painful than immunotherapy-based wart removal injections where the discomfort is usually relatively mild.
The pain experienced during a wart removal injection varies from person to person and depends on individual pain tolerance, the type of injection used, the depth to which it needs to be administered to target the wart effectively, and the specific location and size of the wart. Generally, the injection itself may cause some discomfort, similar to a typical injection or vaccination. You might feel a brief pinch, stinging, or burning sensation when the needle is inserted into the skin. Most patients find the discomfort relatively minor and tolerable, and it typically lasts for just a few seconds.
The price of wart removal injections can vary significantly and depends on several factors, including the number of warts, their size, location on the body, the type of injection used, and the complexity of the treatment. Additionally, the total cost may also be influenced by the number of sessions required, which can vary between individuals and even among different warts on the same person.
As a rough estimate, wart removal injections may range from around $100 to a few hundred dollars or more per injected wart. However, it's essential to keep in mind that this is a general estimate, and the actual cost will differ based on the specific circumstances of the treatment.
When considering the cost-effectiveness of wart removal injections versus other treatments like laser therapy, injections may be more cost-effective, especially for individuals with multiple warts or those with complicated warts located in complex areas. On the other hand, for single isolated warts, destructive treatments like laser therapy might make more financial sense, as they can be a more targeted and efficient treatment option.
Immunotherapy-based wart removal injections are invaluable in certain situations such as those involving complicated warts, multiple warts, or those located in complex and difficult-to-treat areas. The less invasive nature of these injections and their potential to minimize scarring risk and recovery time make them a valuable alternative to destructive treatments. What's intriguing is the possibility of these injections treating not only visible warts but also subclinical warts simultaneously as well as reducing the risk of recurrent warts.
While immunotherapy-based wart removal injections have their place, it's also crucial to be aware of their drawbacks. It's worth mentioning that the use of these injections for wart removal is off-label. The indirect action of these injections, relying on an individual's immune system, means that some warts may be resistant to treatment. The need for multiple sessions (at least 3-6 sessions), the lack of immediate visible changes to the wart and the relatively higher failure rate (15-40%) can be discouraging for some patients. Additionally, the overall cost may be a concern, especially when multiple sessions are required. Transient systemic side effects, such as fever, may occur.
When it comes to destructive wart removal methods, I favour energy-based treatments like lasers over chemotherapy-based wart removal injections. The precision and targeted nature of laser therapy appeal to me, as they reduce the risk of causing damage to healthy skin. Additionally, unlike chemotherapy-based wart removal injections, energy-based treatments do not carry the risk of serious systemic side effects.
In summary, both energy-based destructive treatments and immunotherapy-based wart removal injections have their niche and can be highly effective in the right circumstances.
Wart removal injections offer a promising alternative to traditional destructive treatments. While they’re not suitable for all cases, they can be particularly useful for treating large or multiple warts that have not responded to other treatments.
As always, it’s important to consult with a qualified specialist experienced in treating warts to determine the best treatment option for your specific situation. If you’re struggling with persistent or bothersome warts, consider discussing your options with us today.
Address:
1Aesthetics, Medical & Surgery
#14-90 The Central Tower 1
8 Eu Tong Sen Street
Singapore 059818
Mon-Fri 10 AM to 730 PM
Sat 10 AM to 6 PM
Phone / WhatsApp:
+65 66125173 / +65 84899962
Email:
[email protected]